INNOVATIVE STRATEGIES
FOR
HDC
(High-Definition Care)

The Power to Improve Patient Outcomes
Poor clinical decisions in hospitals lead to missed opportunities to improve patient outcomes, eliminate patient injury, avoid adverse events, reduce costs, and improve patient satisfaction. Poor decisions are rarely intentional, but are driven by high task loads, cognitive biases, knowledge or training deficits, lack of access to critical information, and unintended incentives.
In the movement from volume- to value-based healthcare, good clinical decisions will be critical for financial viability, brand recognition, and success in alternative payment models. Addressing these issues will lead to far better clinical decisions and will markedly reduce the costs of care and drive value into the system.
What is High-Definition Care?
TauSpan High Definition Care Technology was developed by physicians to allow clinicians to make the best possible clinical decisions within their natural workflows by:
- Measuring real-time risks and high-value opportunities in hospitalized patients with machine learning
- Reframing critical clinical decisions using Adaptive Nudge Technology to minimize cognitive biases
- Continual system recalibration to address new issues and sustain improvement
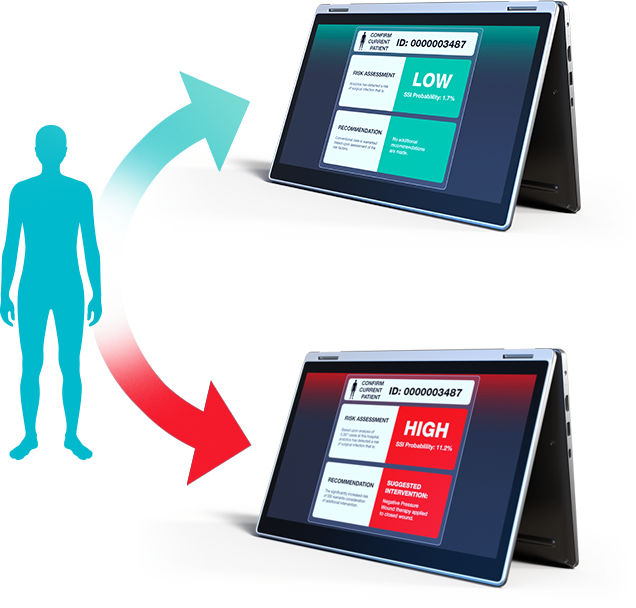
The TauSpan High-Definition Care Platform (HDCP) uses state-of-the-art technology to integrate data from the electronic health record and other organizational data sources while maintaining data privacy, regulatory compliance, data governance, and data integrity. Behind the scenes, HDCP executes real-time machine learning algorithms to identify individual patient risks or opportunities to improve outcomes.
This critical information is then mapped to specific clinical decision points where adaptive nudges are deployed to help frame the critical decisions for the clinician. Because the platform and all of the underlying analytics are fully managed, there is minimal resources required of overextended hospital IT teams.
Example Modules

Surgical site
infections
A proven approach to decrease the prevalence and costs of surgical site infections. HDC-SSI was used to great success at the University of Iowa Hospitals and Clinics (UIHC) where SSI rates dropped 74% over a three year period. At scale that would produce over $1 million in savings for UIHC. HDC-SSI also represents a standardized approach to avoiding pay-for-performance penalties.

Delirium
Current methods of delirium screening are resource intensive, have low sensitivity in practice, and fail to drive appropriate prevention & treatment. Additionally, failure to capture delirium in documentation results in lost reimbursement. HDC-Delirium addresses all of these issues resulting in better outcomes, lower costs, and more appropriate reimbursement

Blood
conservation
Post-operative blood transfusions are costly, with the fully-loaded cost of a unit of blood exceeding $1000. Additionally, transfusions have potentially life threatening complications. HDC-Blood Conservation systematically improves preoperative patient preparation to avoid the need for blood transfusion at the time of elective surgery.
